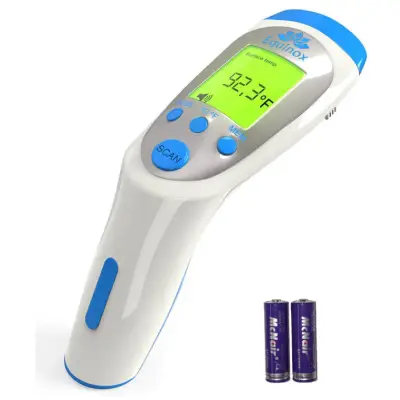
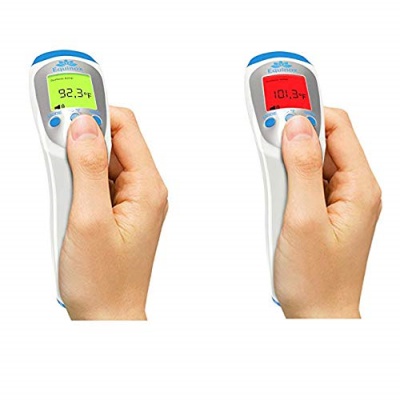
10 Best Baby Thermometers in 2024
At some point in your journey of being a parent, you will experience your child’s first fever. While some fevers won’t cause any harm to your child, others can be a sign of something serious. In order to find out if you need to call your doctor, you will have to take your child’s temperature, especially since your little one won’t be able to tell you they’re not feeling well. If you don’t have a baby thermometer yet, it is time to get one. With our list of the ten best baby thermometers, you won’t have any trouble finding one for your family.
In a Hurry? The test winner after 34 hrs of research
Easy to use
Hard case will keep it clean while traveling
Affordable
Easy to clean

10 Best Baby Thermometers Reviewed
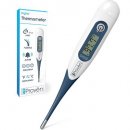
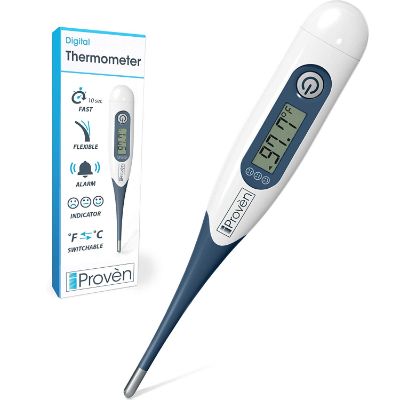
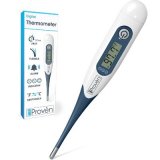
1. iProven Medical Digital
Easy to use
Hard case will keep it clean while traveling
Affordable
Easy to clean
Beep volume is too low
When this baby thermometer with a digital display was completely tested and went through a complete optimizing process that makes sure that this device is the same quality of medical devices that they are using in the hospital. It is a home use thermometer that is able to provide you with the same accurate results and measurements that you would expect from a hospital grade thermometer.
Read moreDesign
The large screen displays the temperature results clearly. Designed with two different beep patterns, you will be able to distinguish if your child has a fever or if a fever is oncoming. The soft flexible tip makes it comfortable for people of all ages to use.
Ease of use
Using this digital baby thermometer is as simple as pressing a button and placing it under the tongue or the rectum. It is a convenient design that supports both uses. The results are displayed within 10 seconds. The display is easy to write and a bonus quick indicator on the side with smileys displays when your little one has a fever.
Accuracy
Designed with an optimized algorithm, you will receive accurate results in no more than ten seconds. One of three smileys will appear to let you know just how serious your child’s temperature is.
Price Range
Priced under fifteen dollars, we find this thermometer to be very affordable as it is easy to use and highly portable.
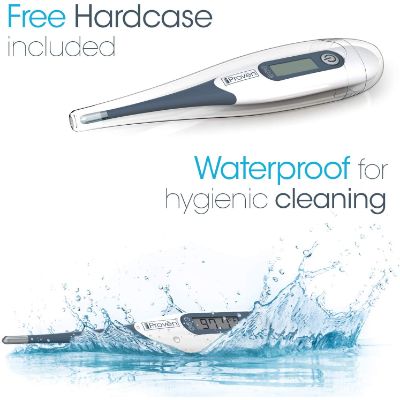
Protection
Along with the thermometer, you will receive a hard case. The case will allow you to travel with the thermometer while keeping it free of dust and debris.
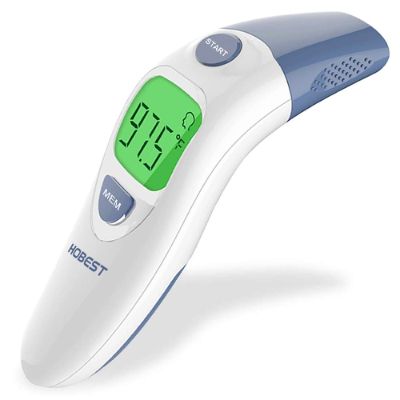
2. Hobest Infrared
Automatic shut off preserves battery life & batteries are included
Allows you to track up to 20 different temperature readings.
Design with four different temperature modes
Easy to use but also includes clear instructions for use
Some reviewers feel the results are inconsistent
When you are responsible for monitoring the health of your family, you want to make sure that you have all the tools that you need. This is a thermometer that features a sensitive and highly precise sensor that is able to provide an instant reading in just a few seconds. It is a professional design and very reliable to be able to meet all the needs of your family.
Read moreDesign
Designed with four different modes, you can take your child’s temperature via their ears or forehead as well as to measure the temperature of their room or milk/water. After thirty seconds, the thermometer will automatically shut off to preserve the batteries. This thermometer gives you the option to measure the temperature in Fahrenheit or Celsius.
Ease of use
Determining if your child has a fever is super easy as the screen will turn red and produce a series of short beeps. Furthermore, the large LCD screen makes it easy for you to read the results clearly. Switch from mode to mode with the simple push of a button. If you seem to be having trouble figuring out how to use it, easy to understand instructions are included in the box
Accuracy
The precise probe and infrared sensor will produce accurate results in 15 seconds.
Price Range
This thermometer is priced just under thirty dollars but with its accurate results and long-lasting battery life, it is worth every penny.
Protection
Track your child’s temperature changes using the data storage feature. This feature allows you to record up to 20 different temperatures.
3. New Generation
Easy to Use
Highly Accurate
Affordable
Equipped with mute reading feature
Many reviewers feel the product is packaged horribly
With a high quality five in one design this thermometer is the perfect device for in your home to be able to measure the temperature of your baby. The device features an infrared scanning that uses the most recent technology with a highly accurate sensor plus a smart ship. It aims to provide the most accurate results to parents allowing them to be about to track fevers at home with reliable devices.
Read moreDesign
Built with a 5 in 1 function design, this thermometer measures the forehead, ears, object temperature, liquid temperature, and room temperature. Save up to thirty-five temperature sets to help you keep track of your baby’s temperature change.
Ease of use
Taking the temperature of your sleeping child is stress-free, thanks to the mute reading feature. The large LCD backlit screen will display your little one’s temperature without releasing a sound and making it easy for you to read the result in the dark. The infrared scanning technology, smart chip, and sensor probe you will receive results quickly.
Accuracy
Recommended by medical professionals, this thermometer has been through countless clinical studies and has been proven as accurate.
Price Range
Priced under thirty dollars, this thermometer is very affordable as it is equipped with the latest technology and produces accurate results quickly.
Protection
This thermometer is perfect for all ages as it has the ability to take your child’s temperature from their ears or forehead. When you’re done using it, simply wipe the probe and tip with an alcohol swab to ensure it is clean for the next use.
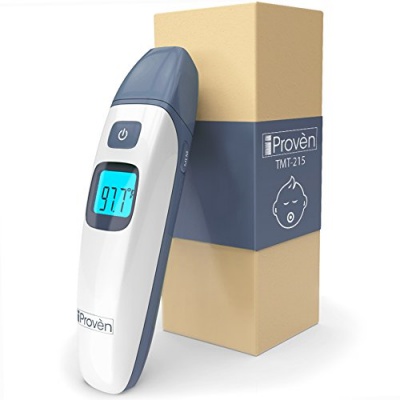
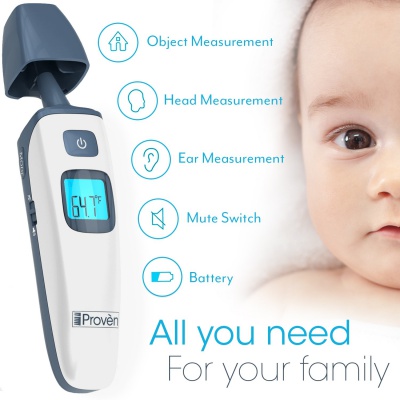
4. iProvèn TMT-215
Ear probe is smooth, easy to clean, and does not need a cover
The three buttons make this an easy thermometer to use: ear, head, and object
The two AAA batteries are included in the packet as is the chamois pouch
All of the features help parents to throw stress out the window
The clear instructions are welcomed by the parents who purchase this item
Taking the cover off of the ear probe is hard for some
Advanced, but still simple, this upgraded thermometer has the same electronics, but with some extras. You can still accurately check temps of children or adults. But now you can also measure the temperature in the room, of the bottle, or the baby’s bath. Measuring temperature in the room is important because the instrument should be acclimated to the air in the room before you use it. This makes it more accurate.
Read moreDesign
One of the features you will love is that you can turn the beep off so don’t have to wake the patient up. That means less anxiety for you and saves you time.
Ease of use
Your baby can sleep through the temp taking process because this thermometer makes it quick, accurate, and even silent.
Accuracy
The digital display will tell you the results by adjusting the light color as well. Parents are loving this instrument because it makes caring for sick loved ones so much easier.
Price Range
This is an upgraded version of a themometer. With a few extra electronic features the additional price is perfect for this all in one and more theromemter. Can work both on children or adults.
Protection
You can also feel comfortable when you put your child in the bath or feed him, knowing he’s not getting burned. The upgrades to this fantastic instrument are very useful when you have a clingy child in hand and you have to do things quickly
5. Metene Infrared
Digital thermometer with accurate readings
Features LED display with backlight
Includes three infrared sensors with German Hyman technology
Easy to use, one button readings
Forehead or ear with no contact design
Steps to which from F to C is difficult to figure out
No probe covers included
Metene has designed a digital thermometer that features an infrared reactor sensor that uses German thermoelectric technology. The sensor is built into the design of the thermometer allowing it to be able to sense ambient temperatures allowing it to be one of the most accurate thermometers on the market. The results are super arcuate and clinically proven to provide the best results each and every time.
Read moreDesign
The thermometer is designed to be used to read temperatures either on the forehead or through the ear. It is easy to be able to switch between the two modes and only features one button on the front of the device. The technology used in the infrared sensor allows the thermometer to not even have to touch the skin. Just aim
Ease of Use
To use this baby thermometer is simple. The first step is to aim or place the thermometer probe that is at the end of the top of the device at the center of their forehead. Once aimed or placed simply press the one button on the front lights and then release. In just a few seconds the device will beep and the temperature will display. It is that easy and no worries with getting an accurate temperature from those little ones.
Accuracy
Built into the device are three upgraded infrared sensors that are able to provide one of the most accurate readings on the market. The sensors provide the device with a precision measurement that is within plus or minus .5 degrees. This is clinically proven to be one of the most reliable measurements and has passed thousands of tests.
Price Range
The price range for this baby thermometer device comes right in at the top of the low range. It is a great device that is able to provide arcuate readings over and over with a price point that is super affordable. This is a thermometer that parents will be thankful to have around when your little one is feeling under the weather.
Protection
Constructed with a user friendly design this baby digital thermometer has been made from an ABS material and features a large display with LED lights. The backlight of the LED display makes it easy to read. On the outside of the display, there is a transparent acrylic that is a panel design that protects the display from scratches and any moisture that would be on the device.
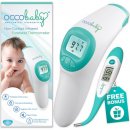
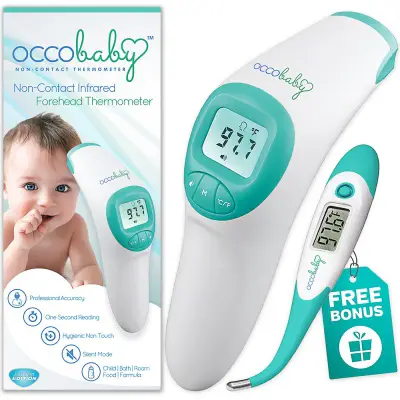
6. OCCObaby Clinical Forehead
Fast Reading
Designed to be a non-contact thermometer
Equipped with a backlight screen & silent mode
Easy to use
Some reviewers feel the backlight is too dim
With the Occobaby Clinical thermometer, you can take the guessing out of judging your child’s temperature. There is also no need to wake your sleeping baby. You can even use it to test the temperature of your child’s food, bath, or formula. Not only is it equipped with a silent mode, but it also has an LCD backlight so you can easily read the screen in the dark.
Read moreDesign
A turquoise fabric bag is included for you to use as a storage bag for the thermometer. The compact size of the thermometer makes it highly portable, thus you can store it in your child’s diaper bag for emergencies.
Ease of use
You won’t be waiting long as the results appear in seconds. You can easily switch between Celcius and Fahrenheit with the push of a button.
Accuracy
You will also receive a rectal thermometer in case you need to double check the temperature reading.
Price Range
Affordable for what you are recieving. Comes with second thermometer just in case.
Protection
This is a no-contact thermometer so you can take their temperature without touching them
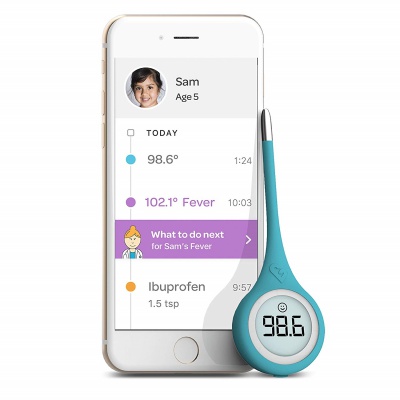
7. Kinsa QuickCare Smart Digital
The pairing of the app and the thermometer is quite easy
The Kinsa can track several kids at once, making storing readings a slam dunk
Shows bubbles on your phone during this process that kids can play with
Buyers reporting a great customer experience when service is needed
The sanitary probe covers are not included in the package
A technically advanced digital thermometer. Who knew? You can use this instrument with its app on your phone or by itself as a regular thermometer, without the tech. Users say this tool gets results very fast, within about 8 seconds, and the app stores the numbers as well as other symptoms to give parents some idea of what may be wrong. Uses a wireless bluetooth connection to your phone. You can enter your child’s symptoms, like a cough or stomach upset.
Read moreDesign
Offering one of the newest types of technology on the market this thermometer is a smart device. The device is designed to be able to connect to an app that has been installed on a smart device that connects to the thermometer. The app logs each temperature and the time that is was taken along with giving suggestions on how to care for the little one. It is the perfect design for the whole family even newborns.
Ease of use
This is a wonderful app for new parents who don’t know what to do, as it gives them the steps. And if you need customer service, they are only a text away.
Accuracy
Add in the medications you are giving, and the timer advises you when it’s time for the next dose. Plus, for your child, he can pop the bubbles on the screen to make this task more fun.
Price Range
Semi-inexpensive. This app will be able to connect right to your phone where you can even enter your child's symptoms and determine their sickness. It's perfect for any new parent to be who might not know what they are doing right off the back.
Protection
The app will guide you through the process of taking care of your little one so you don’t have to worry about what to do next. You can be the caregiver, love your kid, and get her to a point of wellness.
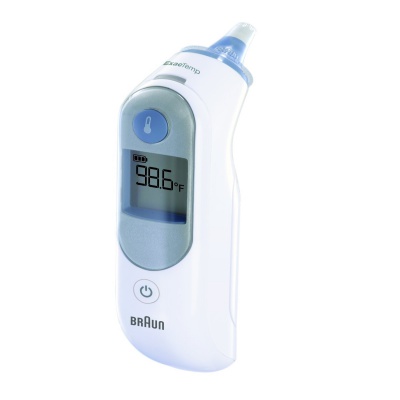
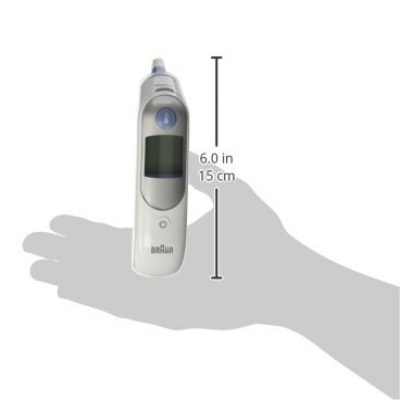
8. Braun Thermoscan
Utilizes a patented, pre-warmed tip for maximum comfort and accuracy.
Used in the medical field by doctors and pediatricians for years.
ExacTemp Technology makes this the most accurate thermometer on the market.
A larger LED screen makes temperatures easy to read.
The flexible tip molds to the ear canal for comfort and accurate readings.
The calibration is very sensitive, so follow the set instructions diligently for a proper set up.
With a patented pre-warmed tip, the Thermoscan5 Ear Thermometer is one of Braun’s most sought after baby thermometers. The pre-warmed tip allows for the more accurate reading of baby’s temperature and has been a mainstay in many doctors’ offices all over the world.
Read moreDesign
It has a large reset button and an even larger LED screen with easy-to-read temperature readings.
Ease of use
Not only is it pre-heated for comfort, but the preheated also aids in overall accuracy. If the tip were cold, they’d be a sort of temperate shock from placing a relatively cold item next to a warmer item. This normal adds variance to temperature readings, but the pre-heated tip takes care of all that guess work.
Accuracy
It features the ExacTemp technology which combines precision placement into the child’s ear with the closest and most accurate temperature readings you can ever find from a baby thermometer.
Price Range
Found in many doctor offices, this thermometer is perfectly priced so that you can use it in the comfort of your own home.
Protection
The tip is also flexible to allow it easy access to any shape of ear canal. To improve the accuracy of the temperature reading, a patented and BPA-free lens filter can be fitted onto the thermometer tip to prevent ear canal temperature fluctuations from affecting the final reading.
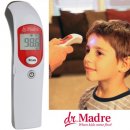
9. Dr. Madre Digital Infrared
This thermometer can talk to you and tell you your child’s temperature.
Features the reading in either Fahrenheit or Celsius.
The speaking function can be muted for bedtime or quiet time.
Can store up to 12 temperature readings for medical purposes or so that you can simply recall your child’s temperature.
This no contact thermometer can simply read the temperature of your child’s forehead without becoming invasive.
Only speaks in English and Spanish.
Being able to care for your little one when they are sick is important. Digital thermometers like this one are perfectly designed to be able to get a quick temperature reading without even having to touch the little one. The design is perfect for being able to accurately monitor their fever with an instant reading and a large display.
Read moreDesign
This Dr. Madre creation actually talks. It voices the temperature reading either in English or Spanish and either in Celsius or Fahrenheit.
Ease of use
It’s also very easy to use as it only requires a click of a button and you now have the most accurate temperature of your baby.
Accuracy
The lack of contact required for use also reduces the amount of germs spread between users. The size of this thermometer allows you to keep it in your child’s nursery or take it on the go.
Price Range
The included case will keep your thermometer in pristine condition so you can use it for years to come.
Protection
At night, the talking function can be turned into silent so as not to disturb baby’s sleep. The thermometer can also be used to take room temperature. It can store 12 temperature readings in its memory.
10. Equinox Digital Non-Contact
Color-changing LCD screen indicates if the temperature is normal, medium, or too hot
Built-in memory records the last 32 readings for easy recall
Utilizes infrared technology to record temperature from 3-5 cm away
Fever alert turns LCD screen red and beeps for any temperature over 100.4 degrees
May have to take temperature multiple times in order to get an accurate average reading
Thermometer can deplete batteries quickly
Versatile and easy to use, the Equinox Digital Forehead Thermometer utilizes infrared technology to allow it to record temperatures from up to 5 centimeters away from your little ones. Room mode also allows you to record the ambient temperature of your baby’s nursery which can be especially useful during months of extreme temperature changes.
Read moreDesign
An easy to read LCD screen display ensures accurate and fast readings. Internal memory stores up to 32 of the last temperatures taken, making it easy to go back and check on how your baby’s fever is progressing throughout the day.
Ease of use
Simply place the device in body mode and rest it against your little one’s forehead to receive almost instantaneous readings that will change color and beep to alert you to a fever.
Accuracy
The surface mode can also accurately measure common objects such as food or formula so that your little one won’t burn their delicate tongue or mouth.
Price Range
This thermometer might be a little bit more expensive. That being said, this thermometer is the all-in one device- that should be in anyone's toolkit.
Protection
The thermometer features a color-changing screen which will change from green to orange to red to quickly indicate whether your little one, the room, or the object you are scanning is too hot.
Criteria Used for Evaluation

Design
Because baby thermometers are vital to the safety and health of children, we were rather strict with our evaluating criteria. As always, safety is the most important aspect of ranking and rating these thermometers. No mercury thermometers or other harmful thermometers are included on this list, and each thermometer has inherent safety features that will be discussed in the Safety section. Accuracy was our second biggest concern. This is because a thermometer is only as good as its rate of accuracy. We included numerous types and models of thermometers with varying rates of accuracy, but all rates are safely above 97%. We discuss these rates in greater depth under the Accuracy section. Finally, our third biggest concern was comfort. It doesn’t matter how accurate or safe a thermometer is if that thermometer isn’t comfortable for the child. For comfort, we specifically looked at the construction and convenience of the thermometer.

Ease of Use
If you are thinking about the same thermometer that were used on us when we were still kids, don’t worry because those glass thermometers are clearly things of the past. Today, everything is digital. Unfortunately, as there are so many products that claim to provide the most accurate temperature readings, it is very important to choose which ones are truly the best.It is for this reason that we came up with this top 10 list of the best baby thermometers. We had to carefully examine each product to determine their accuracy as well as ease of use. We also had to take into consideration whether it will be comfortable for baby as any undue stress can only elevate the temperature even further. We then looked at any sign of certification or recognition from accredited government agencies as well as professional organizations as these are often indications of quality. The different features of the thermometers were also taken into consideration as well as the reviews and feedbacks of parents like us.

Accuracy
Because a thermometer is only as great as its accuracy, we selected thermometers with accuracy rates exceeding 97%. It’s also for this reason that we included numerous types of thermometers. Rectal thermometers are the most accurate measures of temperature, while the mouth and ear method are the least. Though these different types of thermometers have varying accuracy rates, all of the thermometers on this list are greater than 97%. With that being said, no matter how accurate a thermometer can be, it can never be equal to 100% accuracy. The closest you can get to perfect accuracy is in a medical setting.

Price Range
We included various thermometers that are reasonably priced for families. There are even thermometers on our list that can be found in your infants doctors office. Each thermometer is durable, long lasting and a wonderful investment and accesory to have on hand so that you can make sure that your child is safe and healthy at home.

Protection
For the safety of all children, we included numerous types of thermometers on this list. This is because what might work best for newborns might not be safe for older children. For instance, rectal thermometers are great for newborns because they won’t protest as much as an older child would. But oral thermometers, while great for older children, are a choking hazard to babies and newborns. We also abstained from mercury-based thermometers. This is because mercury-based thermometers have been linked to tons of health issues such as nerve damage, mental impairment, and seizures.
Finally, we have comfort. Though this is the last aspect we search for in thermometers, that doesn’t mean comfort is any less important than accuracy or safety. All of the thermometers on this list are designed for both the comfort of the parent and child. The construction of the thermometer is meant to fit comfortably in the hand and also to take the temperature of the child in a comfortable and non-painful way. Even the more invasive options, such as the rectal thermometers, come with features such as guards to ensure comfort and safety.
If you are thinking about the same thermometer that were used on us when we were still kids, don’t worry because those glass thermometers are clearly things of the past. Today, everything is digital. Unfortunately, as there are so many products that claim to provide the most accurate temperature readings, it is very important to choose which ones are truly the best. It is for this reason that we came up with this top 10 list of the best baby thermometers. We had to carefully examine each product to determine their accuracy as well as ease of use. We also had to take into consideration whether it will be comfortable for baby as any undue stress can only elevate the temperature even further. We then looked at any sign of certification or recognition from accredited government agencies as well as professional organizations as these are often indications of quality. The different features of the thermometers were also taken into consideration as well as the reviews and feedbacks of parents like us.
Other Factors to Consider

Safety
Nothing worries Mom and Dad a lot more than feeling baby hot and flushed. Couple this with the knowledge that babies’ immune system and thermoregulation are not yet fully mature and parents can be seen scrambling for answers as to why their babies feel hot. Is it fever? Or is it just Mom and Dad’s apprehension that is making them feel baby is warmer than usual. >There are many reasons why babies have a fever. In most cases, it is often an indication of an infection. Among babies, the most common infections are those caused by viruses and the fever, if any, should readily subside within three days.

Approved by Pediatricians
These often coincide with known seasonal infections like flu season and cold season. However, if the fever persists for more than three days and is unusually high there is a very strong likelihood that your baby has a bacterial infection. This is especially true if the fever is accompanied by other manifestations such as earache, the production of thick and tenacious phlegm, and other signs and symptoms. If you really suspect bacterial infection, make haste as this is usually a medical emergency especially in the first three months of life. The American Academy of Pediatrics says that any 3 month old baby who has a body temperature of not less than 38oC or 100.4oF is deemed to have fever. Doctors, particularly pediatricians, recommend bringing your baby to his or her primary healthcare physician or pediatrician if he or she has fever and any one of the following:
Side Effects
The baby looks very sick, very irritable, and/or unusually sleepy or drowsy
The baby shows other manifestations like severe ear pain, stiff neck, repeated vomiting, unexplained rash, or diarrhea
The baby has had convulsions or seizure
The baby has been in an unusually hot place like an overheated car
The baby has known immune system problems
The baby’s temperature rises to more than 40
The baby’s condition seems to be getting worse
The baby’s fever has persisted for more than 24 hours
It is clear that the temperature we should all be watching out for is the 38oC or 100.4oF mark. As such, we should all be competent in taking the body temperature of our kids. There are four different methods of taking the temperature of children. These include the use of rectal thermometers, axillary thermometer, oral thermometers, and tympanic thermometers. For young infants below the age of 3 months, there is only one method that is considered to be highly accurate-–the rectal method. For infants older than 3 months, tympanic and axillary thermometers are considered acceptable. The use of oral thermometers are generally reserved for older children preferably at least 4 years old.
Effectiveness
Understand that rectal thermometers are the most accurate, albeit quite inconvenient. It provides a very accurate measurement of the body’s core temperature. Axillary, tympanic, and oral thermometers are susceptible to temperature fluctuations of the surfaces upon which the temperature probe is in contact with. These thermometers only provide an estimate of the internal body temperature. Thebgood thing, however, is that these methods provide convenience for Mom and comfort for Baby. Unfortunately you won’t really be able to gauge your baby’s temperature very accurately.
Today’s thermometers are very easy to use because everything is already digital. There is no more need for trying to figure out the mercury readings in old mercury-filled glass thermometers of old. Today, it’s as easy as following the manufacturer’s instructions and keeping the probe as clean as possible. You only need to place the thermometer in the intended body part, wait to hear its beeping sound, and then read the digital display.
It is important to keep a record of your baby’s temperature readings so you will have an idea whether his or her fever is decreasing or not. At the very least, you will have something to show your baby’s pediatrician should you decide to bring your baby to the clinic. This will help in the planning of your baby’s care.
Fever in very young children can scare even the toughest Moms and Dads. That’s why we have listed the top 10 baby thermometers so you will feel more empowered to care for your baby.
Frequently Asked Questions
q: What kind of baby thermometers are there?
There are numerous types of thermometers. Here is a small breakdown of the possible thermometers you can purchase:
Oral Thermometers: These are one of the most common thermometers and they have a rather high accuracy. These thermometers can be placed under the tongue for temperature taking. Though they are not as accurate as rectal thermometers, they are much more comfortable for children to use.
Smart Thermometers: These thermometers can be integrated with phones and other smart devices for constant updates and cataloguing of your child’s health. They usually come with patches that read your child’s temperature, and then the information is sent to a smart device.
Axillary Thermometers: These thermometers do not have to be inserted into your child, but simply placed in the armpit. Though this method isn’t as acute, it’s more comfortable and convenient for both child and parent. Axillary thermometers are usually recommended for sleeping children because the method won’t disturb their rest.
Ear Thermometers: As the name suggests, ear thermometers take a child’s temperature through the ear canal. This method is more accurate than the axillary thermometers but still less accurate than the rectal thermometers.
Temporal-artery Thermometers: The newest kind of thermometer, temporal-artery thermometers use infrared technology to gauge the temperature of a child’s forehead. This method is the most comfortable, but it’s also the most expensive. This type of thermometer is also only for children 3 months and older.
Rectal Thermometers: The most accurate thermometer, rectal thermometer is recommended for children of all ages. However, this thermometer can be the most uncomfortable and dangerous if not used properly. When using the rectal thermometer, please be sure to properly clean and lubricated the device. Rectal thermometers are best for taking extremely sensitive temperatures.
Multi-use thermometers: These thermometers can be used orally, rectally, or axillary. They are one of the least expensive types of thermometers, but they must be thoroughly cleaned after each use. Multi-use thermometers also give some of the most accurate readings, especially when used rectally.
q: Which type of baby thermometer is best for my child?
Which type of baby thermometer is best for your child completely depends on the individualistic needs of the child. Most children do well with all these thermometers with the exception of the rectal thermometer. If your child needs highly accurate temperature readings, then rectal thermometers are the best option. However, rectal thermometers shouldn’t be used past the age of 2 years unless a doctor is performing the reading.
q: When is it appropriate to use a thermometer instead of my hand?
We know that most parents generally use their hands as their first thermometer, and this practice is completely fine. Our hands are very sensitive and can tell us a lot about our child. If your child is showing obvious symptoms, such as vomiting, diarrhea, lethargy, coughing, etc., then you can probably go straight to a handheld thermometer for accurate readings.
q: What are some general safety tips for a baby thermometer?
Some general safety tips for a baby thermometer include: keep the thermometer in a safe and secure location, keep the thermometer clean after every use, never leave your child alone with the thermometer, never take your child’s temperature less than one hour after a bath and less than three hours after a full meal, and take multiple readings whenever possible.
q: What features should I look for in a baby thermometer?
Above all else, consider the needs of your child first before buying a baby thermometer. Your child’s age will ultimately decide which thermometer works best for them. After consulting your child’s age, look at the different types of thermometers. Most parents opt for a multi-use thermometer because they are both accurate and multifunctional.
q: Are rectal thermometers safe?
Yes, rectal thermometers are extremely safe. They also give out the most accurate readings. If you’re concerned with using a rectal thermometer on your child, understand that you don’t have to use a rectal thermometer. Even though they are the most accurate, other thermometers give you pretty accurate readings as well.
q: How can I get my child to sit still enough to take an accurate temperature?
Older children can be reasoned with, so as long as they know what a thermometer does and why it’s important, getting them to sit still should be easy. For younger children, use a thermometer that won’t be disrupted by bodily movements for an accurate reading. Forehead and infrared thermometers are great for fussy or restless babies
q: Can I use a mercury thermometer?
No, mercury thermometers should never be used. Mercury thermometers were popular in the '70s and '80s because we didn’t know the health risks associated with mercury. If you’re using a mercury thermometer, dispose of it properly in favor of a digital one. While mercury vapors are the real danger, we just don’t want to take any risks when it comes to our children.
q: How do I properly clean my baby thermometer?
How you clean a baby thermometer depends entirely on the kind of thermometer you have. For the most accurate methods, clean the baby thermometer in accordance with the written instructions provided. Most of the time, a thermometer can be cleaned with gentle soap and warm water. Some thermometers, in fact, can be placed in the dishwasher for sanitation purposes.
q: How can I tell if my baby thermometer is broken or giving inaccurate readings?
Sometimes, it can be rather difficult to tell if a baby thermometer is giving you the wrong reading. If the baby thermometer is flashing a digital reading that seems either way too high, or way too low, then it most likely is giving you an incorrect reading. Also, if you notice the LED screen petering out or flashing with a pair of fresh batteries, then it’s time to invest in a new one.
Sources
- , How to buy a thermometer, Blog
- , Baby Thermometer Safety, Article
- , Thermometer basics: Taking your child's temperature, Health Journal
- , Mercury and health, WHO Info Article
- , Fever advice, Article